|
|
Josep Llados, Ernest Valveny, & Enric Marti. (2000)." Symbol Recognition in Document Image Analysis: Methods and Challenges" In Recent Research Developments in Pattern Recognition, Transworld Research Network, (Vol. 1, 151–178.).
|
|
|
|
Josep Llados, Ernest Valveny, Gemma Sanchez, & Enric Marti. (2002). "Symbol recognition: current advances and perspectives " In Dorothea Blostein and Young- Bin Kwon (Ed.), Graphics Recognition Algorithms And Applications (Vol. 2390, pp. 104–128). Lecture Notes in Computer Science. Springer-Verlag.

Abstract: The recognition of symbols in graphic documents is an intensive research activity in the community of pattern recognition and document analysis. A key issue in the interpretation of maps, engineering drawings, diagrams, etc. is the recognition of domain dependent symbols according to a symbol database. In this work we first review the most outstanding symbol recognition methods from two different points of view: application domains and pattern recognition methods. In the second part of the paper, open and unaddressed problems involved in symbol recognition are described, analyzing their current state of art and discussing future research challenges. Thus, issues such as symbol representation, matching, segmentation, learning, scalability of recognition methods and performance evaluation are addressed in this work. Finally, we discuss the perspectives of symbol recognition concerning to new paradigms such as user interfaces in handheld computers or document database and WWW indexing by graphical content.
|
|
|
|
Aura Hernandez-Sabate, & Debora Gil. (2012). "The Benefits of IVUS Dynamics for Retrieving Stable Models of Arteries " In Yasuhiro Honda (Ed.), Intravascular Ultrasound (pp. 185–206). Intech.
|
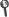
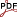
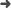
|
|
|
Debora Gil, Oriol Ramos Terrades, & Raquel Perez. (2021). "Topological Radiomics (TOPiomics): Early Detection of Genetic Abnormalities in Cancer Treatment Evolution " In Extended Abstracts GEOMVAP 2019, Trends in Mathematics 15 (Vol. 15, 89–93). Springer Nature.
Abstract: Abnormalities in radiomic measures correlate to genomic alterations prone to alter the outcome of personalized anti-cancer treatments. TOPiomics is a new method for the early detection of variations in tumor imaging phenotype from a topological structure in multi-view radiomic spaces.
|
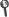
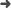
|
|
|
Carles Sanchez. (2014)." Tracheal Structure Characterization using Geometric and Appearance Models for Efficient Assessment of Stenosis in Videobronchoscopy" (F. Javier Sanchez, Debora Gil, & Jorge Bernal, Eds.). Ph.D. thesis, Ediciones Graficas Rey, .

Abstract: Recent advances in endoscopic devices have increased their use for minimal invasive diagnostic and intervention procedures. Among all endoscopic modalities, bronchoscopy is one of the most frequent with around 261 millions of procedures per year. Although the use of bronchoscopy is spread among clinical facilities it presents some drawbacks, being the visual inspection for the assessment of anatomical measurements the most prevalent of them. In
particular, inaccuracies in the estimation of the degree of stenosis (the percentage of obstructed airway) decreases its diagnostic yield and might lead to erroneous treatments. An objective computation of tracheal stenosis in bronchoscopy videos would constitute a breakthrough for this non-invasive technique and a reduction in treatment cost.
This thesis settles the first steps towards on-line reliable extraction of anatomical information from videobronchoscopy for computation of objective measures. In particular, we focus on the computation of the degree of stenosis, which is obtained by comparing the area delimited by a healthy tracheal ring and the stenosed lumen. Reliable extraction of airway structures in interventional videobronchoscopy is a challenging task. This is mainly due to the large variety of acquisition conditions (positions and illumination), devices (different digitalizations) and in videos acquired at the operating room the unpredicted presence of surgical devices (such as probe ends). This thesis contributes to on-line stenosis assessment in several ways. We
propose a parametric strategy for the extraction of lumen and tracheal rings regions based on the characterization of their geometry and appearance that guide a deformable model. The geometric and appearance characterization is based on a physical model describing the way bronchoscopy images are obtained and includes local and global descriptions. In order to ensure a systematic applicability we present a statistical framework to select the optimal
parameters of our method. Experiments perform on the first public annotated database, show that the performance of our method is comparable to the one provided by clinicians and its computation time allows for a on-line implementation in the operating room.
|
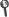
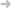
|